If you live with chronic pain, the notion of “good days” and “bad days” is very different from your neighbor’s. It isn’t about missing a deadline at work, or the dry cleaner ruining your favorite suit.
It begins with the morning
A good day is one in which you can get up and move around for a little bit of time, in which someone’s smile actually pierces the weight and remove in which you live each hour.
 A good day is when some sort of pain management technique – medication, stretching, meditating – actually achieves its goal.
A good day is when some sort of pain management technique – medication, stretching, meditating – actually achieves its goal.
A good day is when you live an echo of a former life, your life without acute pain that you must manage, without performance for the benefit of those you love and those you work with.
And of course, a bad day is quite the opposite.
You’re angry. You’re frustrated. You’re probably depressed. No amount of medication seems sufficient. Movement – even slight – sends searing pain through your back or your limbs.
You feel like a prisoner in your bed, your room, your home.
You are a prisoner in your own body, and those you love and who love you are weary and frustrated with their inability to help.
Fibromyalgia
Fibromyalgia is a particularly insidious example, one which I lived with for years. It is often an undiagnosed illness, and medical professionals used to deem it psychosomatic. I can’t tell you how many times I heard “you’re tired and I suspect that you’re depressed. It’s the depression that’s causing the pain. There is no physical reason for it.”
I was dismissed by the profession that was supposed to help. Told that my pain wasn’t “real.”
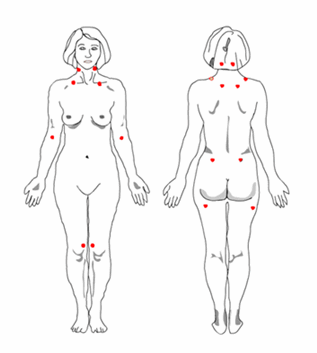
Try waking with thrumming ache in the back of your neck, your collar bones, your shoulders, your hips, your legs. There is literally no movement that doesn’t hurt.
I was tested for everything from lupus to rheumatoid arthritis, as every muscle seemed to throb from somewhere so deep inside that no heat or ice could reach it.
 Imagine being so physically exhausted that walking from the bed to the bathroom is like moving through a wall of rock. Only the wall of rock is your own body.
Imagine being so physically exhausted that walking from the bed to the bathroom is like moving through a wall of rock. Only the wall of rock is your own body.
Imagine pretending that everything is fine – through a screen of pain you dull with a glass of wine or as many over-the-counter pain killers as your body can tolerate. All so you can lift your child or manage to make it to the grocery store and back. So you can carry on a conversation with your spouse, who doesn’t want to hear that you don’t feel well, and who doesn’t believe it anyway.
Try thinking back to when you did feel well, and being unable to recall what that felt like. You know it has been years – three, five, you’ve lost count.
I was fortunate.
Eventually, quite by accident, I found a doctor who said “I think I know what is wrong with you, and I think we can improve things.”
As it turned out, I suffered from Restless Leg Syndrome, which required an overnight stay in the hospital (for a sleep study), and subsequent medication – in a very small dose. According to the National Institutes of Health, Restless Leg Syndrome is a lifelong condition for which there is no cure. But it is very manageable. What is destructive, in retrospect, are the years before diagnosis when you do not know what is wrong. The blur of months without answers or hope – and all the ensuing health problems that can be dramatic and life altering – that result from insufficient and interrupted sleep.
When my RLS was diagnosed and addressed, the fibromyalgia lessened and ultimately disappeared – along with a host of other sleep-deprivation issues that were quite severe. I quickly adapted to some necessary lifestyle changes, which keep me functioning fine.
Apparently, some studies have shown that there are associations between Restless Leg Syndrome and Fibromyalgia, as was my case.
More recently, I’ve had recurring lower back pain (from an old injury), and for the past two and a half years I have lived with chronic pain in one arm, shoulder, and knee – the result of a car accident. I tried physical therapy (which worsened the condition), and I’ve tried living with my body as it is. I stretch, do very gentle exercises as I can, and that works better for me.
Good days and bad days
There are days when the pain is severe, particularly in my shoulder and arm; other days when it’s just annoying. In both instances, it interferes with my life in ways that I don’t talk about. Oh, it’s simple, everyday things – changing the sheets on my bed or cleaning up in the kitchen – painful. Writing in my journal by hand – the movement to my shoulder as I move my hand across the page – painful. Carrying groceries, even packed light, from the car into the house. Painful. Reaching into the sink to rinse dishes. Painful.
There is the loss of activities I loved, and also that helped keep me fit – tennis and swimming – now out of reach. Out of reach forever? I don’t know. I hope not, but out of the picture for now.
Work accommodations – unofficially
More troublesome when it comes to daily living is the fact that I need special accommodations when I am in an office environment (due to my right arm). They aren’t a big deal, but who doesn’t hesitate to ask for any seemingly special treatment in today’s job market?
And I have no “special needs” or ADA (Americans with Disabilities) status, officially. These are tough economic times – when I go for a job or project interview, I certainly don’t mention that simple things like using a desktop computer and mouse will put me in pain after an hour or two.
I just deal.
The pain is steady and tiring, but I can usually put it out of my mind. For a few hours, anyway. Eventually, if I can, I request a laptop which I can maneuver more easily, reducing the stress on my right arm and shoulder.
Chronic Back Pain
If chronic back pain is something you live with, I don’t have to tell you that your entire body is impacted. Getting out of bed in the morning – stiffly – is sharp contrast to the peacefulness of sleep. If you are able to sleep.
For me, sleep is a blissful time; in my dreams, I can lift a child, without rippling pain in my shoulder and forearm. I can dance as I once did. I can walk up and down hills for miles, without pain in my knee. I can make love and nothing hurts. I swim with full, arcing strokes, and I hit a tennis ball and run with abandon.
In my dreams I am free and whole, and grateful for those dreams, for their renewal of energy, for the pleasure of being physical – without pain.
But waking is a shock.
Humor helps
While a sense of humor may come and go, there’s plenty of truth to the adage that laughter helps. It lightens things up, and puts others at ease which in turn helps you be at ease if you’re in pain.
I travel for some of my writing ventures, infrequently. Some of that travel is overseas, which entails hours at the airport beforehand, dragging a laptop (oh my shoulder!) along with luggage, and many hours of sitting in cramped quarters to cross an ocean. I bring a small heating pad in my carry-on; I can’t use it on the plane, but I find a plug and use it to wait, right up until boarding. I alternate between heat on my arm and heat on my back.
When I get a raised eyebrow (I’m sometimes propped against a post for support, on the floor), I just smile and say “Nothing serious. Wild sex.”
Sometimes I get a chuckle, sometimes I get another raised eyebrow. But more often than not, my own smile and lightness of tone puts others at ease and may even start up an interesting conversation.
Perspective
If you live with chronic pain, remember that others don’t. Give them a break. They can’t possibly understand what it’s like.
It’s important to remember that if you haven’t lived it, you can’t imagine it. Even the most sympathetic and compassionate friend or partner can’t fully grasp what it’s like to be inside your body. And imagine how tiring and frustrating it must be for them, unable to share what they’d like with you, and feeling guilty for being healthy.
What if you’re the caretaker or loved one of someone in chronic pain?
If you care for someone in chronic pain, here are a few thoughts and personal stories.
I have a friend who underwent back surgery years ago. It never properly healed, or rather, it healed to the extent that it will. He endured months of physical therapy, pain management medication and procedures, and followed every doctor’s order. He still lives with considerable pain. He handles it more gracefully than I ever could.
Pain has cut short participation in local theater, cultural activities, and entertaining. Holidays with the family are not only exhausting physically, but more so, for the smile he wears so they don’t feel guilty about being healthy. So he is less of a burden to those he loves. Travel for him is excruciating. Picking up his grandchild is not easily done, and always carries a price.
But worst of all, relationships shift. Sexuality, all too often, drifts away, along with all the emotional benefits of intimacy and well-being.
 I have also lived this experience – the years that Fibromyalgia had me aching on good days, and bedridden on bad days.
I have also lived this experience – the years that Fibromyalgia had me aching on good days, and bedridden on bad days.
My husband traveled, and wasn’t around to see the worst of it. He was among those who said “it’s all in your head,” adding to the emotional distance between us.
It was my older son, then 6 years old, who picked me up off the floor when I crumpled, who helped me to bed, whose smile and optimism – along with his little brother’s – kept me going.
Because I wanted my marriage to be calm and “healthy,” I pretended. As much as I could. I was a loving partner to the extent that I was able. I delivered the demeanor expected, no matter how many Tylenol or Advil it took to do so.
More painful than the “pain” was denial, by the person I loved and who was supposed to love me. Denial that there was anything wrong, and the resulting diminishing of the “self” – my perception as active and engaged in the world, as deserving of being valued, as able to contribute, and as a sexual being worthy of touch.
A person in chronic pain remains a full person inside, and requires your understanding when it comes to family outings, fatigue from routine work, mood swings, traveling, lifting a child – and of course, sharing a sex life.
Share a sex life, if possible
I’m all for creativity – in everything! And acts of love are no exception. Think of this as your opportunity to experiment. Eroticism begins in the mind – with images, words, aromas, music, a whisper, a surprise…
Even with physical challenges, you still have options. And if you care for someone who lives with chronic pain, or you live with chronic pain – that most intimate connection – however it is accomplished and to whatever extent – will do a world of good, for both of you.
Please remember – I am not a health care professional or a therapist. These are personal experiences and the experience of friends.
Opportunities for Tender Touch
Something as simple as massage can be both soothing and sexual.
Massage followed by localized sexual contact – whether dealing with a man or a woman – can lessen the need for significant movement, while still providing a great deal of pleasure. In other words, use your hands or mouth on your partner.
Inspired positioning can also be a solution. For a man with back problems, a sitting position, in a comfortable chair with good support (leaned against a heating pad if that assists and is doctor-approved), will allow your partner to do the rest – again, with the hand or the mouth.
If your partner is agile enough (and the chair sufficiently sturdy!) she may seat herself facing you, and use the strength in her legs to provide a very engaging sexual experience – a position for everyone to enjoy!
If the woman suffers from chronic back pain, she may lie on a heating pad (with some sort of clothing between her skin and the source of heat to prevent burns), propped in a way that there is little to no pain.
Her partner may be able to enjoy a variety of playful and pleasurable activities for both, including the visual stimulation of seeing her, and his enthusiastic response.
Get Creative!
Play with food! Play with scrabble tiles! Cool surfaces and varied textures produce delightful responses. Sexual contact is at least as much about the mind’s willingness to let go and enjoy emotional connection. Living and loving with chronic pain doesn’t mean giving up fun.
And let’s not forget the delights and power of kissing.
Lips are extraordinarily sensitive, and the kiss remains one of the most romantic and intimate gestures there is. Physical closeness – lying together, kissing – expresses so much more than sexuality. It communicates love, tenderness, understanding. And don’t leave it to the lips alone. Hold hands, touch your partner’s face.
Don’t forget about fingers and fingertips as well as nipples – both a man’s and a woman’s. So many parts of the body are sensitive to pleasure, without requiring a great deal of movement on the part of the partner who otherwise might be in pain.
Medications and Sexual Performance
Superstud performance is not a requirement for intimacy. We have our prime, and we have our autumn. If pain or medications reduce sexual capacity, creativity can jazz up the evening with foreplay, wordplay, and pleasuring the other.
Pain breeds depression. And isolation reinforces it. Loss of sexuality and simple acts of affection will worsen the situation. Not only for the one who suffers from chronic pain, but for the partner, and the relationship.
Each scenario will differ, of course. But being trapped in your own body that refuses to work as it once did is infuriating, draining, and potentially destructive to all relationships – professional and personal.
 I have no solutions. Only my own stories – years of doctors, visits to pain management specialists who offered fistfuls of capsules and invasive procedures, a spouse who didn’t care or didn’t believe, and who ultimately became an ex-spouse. Even now, when chronic pain rears up – the reality of knowing that a rich sex life is possible with a creative partner eases my worries about the future. And that means a good day. A lot of good days.
I have no solutions. Only my own stories – years of doctors, visits to pain management specialists who offered fistfuls of capsules and invasive procedures, a spouse who didn’t care or didn’t believe, and who ultimately became an ex-spouse. Even now, when chronic pain rears up – the reality of knowing that a rich sex life is possible with a creative partner eases my worries about the future. And that means a good day. A lot of good days.
I consider my situation to be an “inconvenience.” I manage as I need to, and it works for me. When I need to withdraw from the world at large – to the extent that a single mother can – I do.
But there are no Pollyanna answers, and trite advice like “think positive thoughts” or “just put it out of your head” simply doesn’t cut it. Especially on the bad days.
What thoughts would I like to leave you with?
Communication is essential. Talk or write. Share stories with others who live with acute pain, and may have suggestions for managing it, as well as providing a safe place to vent. That’s huge. You need to be able to express your anger.
You may also get assistance in managing other relationships – with spouses, friends, children, parents, colleagues – and your medical professionals and caretakers.
Just because we live in pain – and sometimes we can’t help but show it – doesn’t mean we are any less worthy of your love, your respect, or your touch. We may need creative solutions to logistics, but we are still here. And touch, handled in a caring way as well as sexual, is all the more important. It is humanizing. It reminds us, even if momentarily, that we are still ourselves.
And the choir says Amen.
The thing that gets me is hearing “one day when you’re better and over this.” There is no getting over this – this is what it is. That and the pain makes me so hard to live with. I remember telling my boss “fine, I can do that project but I already know it’s going to take about 5 darvocet to get through it.” Telling my kids “I don’t care what you do but shut up because my head is killing me.” Pain makes me angry and mean. Planning trips is hard, doing things with the kids is hard – they want to ride the train at the mountain? Pop a couple of darvocet just to be able to smile and say ok. I can’t predict when it’s going to get bad or when I have a great day. It just is what it is and I have to be prepared.
The unpredictability is one of the hardest parts. It makes parenting extremely challenging, and planning almost impossible. You hope for the best and do the best you can.
I don’t know how old your children are, but my own, I think, are growing up with more compassion than most. My oldest son helped me through those long years of Fibromyalgia, before the RLS was diagnosed and things improved. I don’t know if he’ll retain those memories or not. I had to get very creative as a single parent just to get “normal things” done. I had to ask for help – which was difficult for me – particularly with everyone saying “you’re fine.” And only my kids and I knew that I wasn’t.
Hang in. You aren’t alone.
YES – exactly. Good days are few and far between, and I no longer remember what it’s like to have a day without pain, or a nite I don’t need hot pads and hypnosis cd’s to be able to sleep (if sleep happens at all.) It’s amazing to read something by someone who really understands what it’s like. Thank you.
Thank you for sending this to me. It’s all new enough to me… that a simple flash of recognition is enormous comfort. And the image that held me tonight was that of sleep being bliss. It is. Bliss. (Assuming I find sleep.) I can rest. My mind stops worrying about my body. I dream of running for miles and miles and feeling the wind in my hair. That is what I will think of as I fall asleep tonight. (Well, that and beautiful writers whom I’ve only just found.) Thank you for sharing your experience. It helps.
I just found your blog and love it. I too suffer from fibromyalgia and other chronic conditions. Writing and humor are my coping mechanisms. Thanks for a great article.
What a great blog you have! So glad you found me. Welcome.